Epithelioid mesothelioma is a subtype of mesothelioma cancer and is caused by asbestos. It accounts for roughly 70% of all mesothelioma cases. Epithelial mesothelioma cells stick together and spread slowly, making them easier to treat. We can help eligible veterans with epithelioid mesothelioma pursue military benefits, treatment, and compensation.
What Is Epithelioid Mesothelioma?
 Epithelioid mesothelioma (also called epithelial mesothelioma) forms when epithelial cells, which line the inner and outer surfaces of your body, become malignant (cancerous) after asbestos exposure. Many U.S. veterans and civilians have been affected by this cancer.
Epithelioid mesothelioma (also called epithelial mesothelioma) forms when epithelial cells, which line the inner and outer surfaces of your body, become malignant (cancerous) after asbestos exposure. Many U.S. veterans and civilians have been affected by this cancer.
Epithelioid Mesothelioma Quick Facts
- About 70% of mesothelioma patients have this type, according to the American Society of Clinical Oncology (ASCO).
- Approximately 700 U.S. veterans are diagnosed with epithelial mesothelioma per year.
- Epithelial tumors can form in the lining of the lungs, abdomen, heart, or testes.
- Epithelioid mesothelioma cells are oval or cube-shaped. They divide rapidly but stick to one another.
- This type is more easily treated than the other mesothelioma cell types (biphasic and sarcomatoid).
Malignant epithelioid mesothelioma patients live for almost 3 years on average if they get treatment, and some live even longer.

If you or a U.S. veteran you love has epithelioid mesothelioma, the Mesothelioma Veterans Center stands ready to help you pursue benefits from the U.S. Department of Veterans Affairs (VA), medical care, and compensation.
Get our Free Veterans Packet to see all the ways we can assist you after an epithelial mesothelioma diagnosis.
Epithelioid Mesothelioma Causes
All types of mesothelioma are caused by asbestos exposure. Asbestos was used in many occupations since it was a good construction material and insulator.
Breathing in or swallowing asbestos fibers can lead to epithelioid mesothelioma cancer 10-50 years later.
You’re at a higher risk of any type of mesothelioma if you served in the U.S. military before the early 1980s, since all branches used asbestos-containing products in bases, vehicles, and ships.
Epithelioid Mesothelioma Symptoms
Symptoms of epithelioid cancer typically start off mild but worsen over time. As a result, epithelioid mesothelioma could be mistaken for a more common illness like the flu.


Epithelial mesothelioma symptoms include:
- Chest pain and a cough
- Loss of appetite
- Lump on the chest wall beneath the skin
- Nausea or vomiting
- Pleural effusions (fluid buildup in the lung lining)
- Shortness of breath
- Unexplained weight loss
See a mesothelioma doctor if you have any epithelial mesothelioma symptoms and were exposed to asbestos during your military service or at a job. By doing so, you can get diagnosed and treated promptly.
Mesothelioma Epithelioid Diagnosis
To diagnose malignant epithelial mesothelioma, your doctors will conduct a physical exam and take note of any symptoms you have.
They’ll then look for tumors in your body using imaging tests like:
- CT (computed tomography) scans
- MRI (magnetic resonance imaging) scans
- PET (positron emission tomography) scans
- X-rays
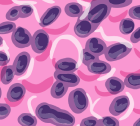

If doctors find signs of cancer on these scans, they’ll order a biopsy to remove a fluid or tissue sample for review under a microscope. This test is the only way doctors can confirm an epithelial mesothelioma diagnosis.
Using Immunohistochemistry to Diagnose Epithelioid Mesothelioma
Pathologists (doctors who study cell and tissue samples) may use immunohistochemical staining to confirm a diagnosis. This involves ‘staining’ a tissue sample to check for substances that indicate cancer and can help prevent misdiagnosis.
Doctors often look for the protein calretinin on stains, which is present in 95% of epithelioid mesothelioma cases.
A 2024 report in The American Journal of Surgical Pathology also noted that staining for secreted protein acidic and cysteine-rich (SPARC) could help distinguish epithelial pleural mesothelioma from lung cancers like adenocarcinoma.
Epithelioid Mesothelioma Types
Doctors can classify epithelioid mesothelioma into different types depending on where tumors form in the body.
Types of epithelial malignant mesothelioma include:
- Epithelioid pleural mesothelioma: This is the most common type. Cancerous epithelial cells form in the lining of the lungs (pleura) and then spread to other parts of the body.
- Epithelioid peritoneal mesothelioma: Cancer cells and tumors develop in the lining of the abdomen (peritoneum). Peritoneal epithelioid mesothelioma is rarer than pleural epithelioid mesothelioma but easier to treat.
- Rare types: Epithelioid mesothelioma can also develop in the lining of the heart (pericardium) or testicles (tunica vaginalis) in very rare cases.
Doctors can determine which mesothelioma epithelioid type you have at the time of diagnosis and use this to develop the best possible treatment plan.
Subtypes of Epithelioid Mesothelioma
There are several subtypes of epithelioid mesothelioma. Which subtype you have can affect your health outcome as some are easier to treat than others.
Adenomatoid Mesothelioma
This accounts for about 5% of all cases of malignant pleural mesothelioma. It needs to be distinguished from benign (noncancerous) adenomatoid tumors.
Cystic Mesothelioma
This type is usually found in cases of peritoneal epithelial mesothelioma that affect women. It is usually benign (noncancerous), so patients usually live longer.
Deciduoid Mesothelioma
Fewer than 5% of patients have deciduoid mesothelioma, according to a 2022 study. This subtype has a poor health outlook, but treatments may still help.
Solid Mesothelioma
This subtype forms in nest or sheet-like patterns. It is the most common subtype according to a 2025 Modern Pathology report, accounting for 40% of cases. A Histopathology study found that patients with this type had an average overall survival time of more than 1 year.
Tubulopapillary Mesothelioma
This is the second-most common subtype, making up about 35% of cases, according to the 2025 Modern Pathology study. It has cube-shaped cells and grows slowly. Patients with this subtype lived for nearly 2 years on average in a Histopathology study.
Well-Differentiated Papillary Mesothelioma
This is a very rare subtype. Most cases are considered benign and the cells spread slowly. However, a recent Modern Pathology report found that some cases could be cancerous.
A mesothelioma specialist can determine which epithelial mesothelioma subtype you have, if any, when reviewing a biopsy under a microscope.
Epithelioid Mesothelioma Prognosis
Epithelioid type mesothelioma often has a better prognosis (health outlook) than sarcomatoid or biphasic mesothelioma, with many patients living for several years after a diagnosis.
Mesothelioma prognosis is measured using life expectancy and survival rate. Find prognosis information for epithelioid mesothelioma below.
Epithelioid Mesothelioma Life Expectancy
Mesothelioma life expectancy is the average amount of time patients live after a diagnosis. The life expectancy for epithelioid patients is nearly 3 years or more with treatment.
Get our Free Veterans Packet to learn how we can help you access treatments to improve your life expectancy.
Epithelial Mesothelioma Survival Rate
Survival rate is the percentage of patients still alive a certain number of years after diagnosis.
The 2-year epithelial mesothelioma survival rate is 45% and the 5-year survival rate is 14% with surgery, according to a 2022 review National Cancer Database (NCDB) patient outcomes.
By comparison, the 2-year survival rate for sarcomatoid mesothelioma is 15% with treatment.
Epithelioid Mesothelioma Treatment
Surgery, chemotherapy, immunotherapy, and radiation therapy are common epithelioid mesothelioma treatments that help patients live longer. Learn about epithelial mesothelioma treatments that could potentially improve your prognosis.
Epithelioid Mesothelioma Surgery
Doctors may use mesothelioma surgery to remove tumors if there is no metastasis (cancer spread through the body).
Epithelioid mesothelioma surgeries include:
- Extrapleural pneumonectomy (EPP): Used to treat pleural mesothelioma by removing the tumors, the lung closest to the cancer, and the pleura. Epithelial patients treated with an EPP lived for 22 months on average in a 2022 Translational Lung Cancer Research report.
- Pleurectomy with decortication (P/D): Also used for pleural mesothelioma, but only the pleura and cancer are removed (both lungs stay intact). Epithelial patients who received a P/D and chemotherapy lived for over 38 months on average in the 2022 report above.
- Cytoreduction with HIPEC: Used to treat peritoneal mesothelioma by removing cancer tumors and then applying heated chemotherapy. The 5-year survival rate was 42% and the average life expectancy was 38.4 months in a 2022 study.
“The epithelial subtype, which is the most common, is the one that is the most amenable to surgical intervention.”
– Dr. Joseph Friedberg, mesothelioma specialist
Call (877) 450-8973 to learn if surgeries could be a part of your epithelioid mesothelioma treatment plan.
Chemotherapy
Chemotherapy medications like pemetrexed and cisplatin can destroy epithelioid cancer cells. Epithelial mesothelioma patients treated with chemotherapy lived for 15.8 months on average in a 2022 Translational Lung Cancer Research report.
Immunotherapy
Immunotherapy helps the immune system fight cancer. Pleural epithelioid mesothelioma patients lived for 18.2 months when treated with immunotherapy according to 2022 NCDB data.
Other Treatment Options for Epithelial Mesothelioma
Doctors at top cancer centers can use other treatments or combinations of therapies to improve survival and reduce epithelioid mesothelioma symptoms.
These include:
- Clinical trials: These test new treatments or combinations of therapies. A study started in December 2024 is investigating how a new drug, ISM6331, can help pleural epithelioid mesothelioma patients live longer.
- Multimodal therapy: Multiple treatments are used to improve survival. Women with epithelial mesothelioma who received an EPP, radiation, and chemotherapy lived for 70 months (nearly 6 years) on average, according to a Journal of Thoracic Oncology study.
- Palliative care: This focuses on easing pain and symptoms. A 2021 Chest report noted how palliative chemotherapy and radiation helped a U.S. Navy veteran with stage 3 epithelioid mesothelioma live for 1 year after his diagnosis.
- Radiation: This uses beams of energy to kill cancer. In a 2021 Communications Biology study, epithelioid patients who received radiation and surgery lived for 36 months on average.
Use our 14 Questions to Ask Your Doctor Checklist to find out which treatments may be best for you after an epithelioid mesothelioma diagnosis.
Get Help for Epithelioid Mesothelioma
If you or someone you love is a U.S. veteran fighting mesothelioma, know you’re not alone and that we may be able to help you.
The Mesothelioma Veterans Center will walk with you through your diagnosis and assist in any way we can.
Here are the next steps to take if you have epithelioid mesothelioma:
- Get our Free Veterans Packet: This guide can help you understand your epithelioid mesothelioma diagnosis and medical options.
- File or increase VA benefits: Mesothelioma VA benefits are worth over $4,000 as of 2025. We can help you file for or maximize your benefits.
- Find treatments: Work with our caring and dedicated nurses to find the best doctors and treatments for your case.
- Get additional compensation: We recently secured $8.26 million for an epithelial patient, and millions could be available to you too with our assistance.
Call (877) 450-8973 to learn about all the ways we can help you or a loved one.
Epithelial Mesothelioma FAQs
Is epithelioid mesothelioma curable?
There is no official cure for epithelioid mesothelioma yet, but veterans and civilians with this cancer might live for many years depending on the treatments they receive.
Surgery, chemotherapy, and other treatments can all help improve life expectancy.
What is the life expectancy of someone with epithelioid mesothelioma?
The average epithelioid mesothelioma life expectancy is nearly 3 years with treatment.
If doctors diagnose the cancer before it has spread, they’re often able to use aggressive treatments like surgery and chemotherapy to help patients live longer.
What is the survival rate for epithelioid mesothelioma?
Pleural epithelioid mesothelioma patients had a 2-year survival rate of 45% and a 5-year survival rate of 14% when treated with surgery, according to a 2022 review of National Cancer Database (NCDB) patient outcomes.
How long you’ll live depends on your overall health, cancer stage, treatment plan, and other factors following a diagnosis.
What is the difference between epithelioid vs. sarcomatoid mesothelioma?
Epithelioid malignant mesothelioma is the most common cell type and is easier to treat since cells stick together. The cells are shaped like ovals or cubes.
Sarcomatoid mesothelioma is the rarest and hardest to treat. These cells are shaped like spindles, so they don’t stick together as easily and can spread rapidly through the body.
“The best patients are going to be probably the epithelioid types,” mesothelioma specialist Dr. Edward Levine said in a recent interview. “Sarcomatoid patients are not great candidates for surgeries like cytoreduction and HIPEC.”
We can help you find top doctors for any type of mesothelioma. Contact us now to get started.
What are the stages of epithelioid mesothelioma?
There are four epithelioid mesothelioma stages. The lower the stage, the easier the cancer is to treat.
The stages of pleural epithelioid mesothelioma are:
- Stage 1: This is the least advanced stage, and patients have the best prognosis since the cancer will be easier to treat with surgery.
- Stage 2: The cancer has started to spread in stage 2, but doctors can often effectively remove tumors by using surgery.
- Stage 3: Patients may not qualify for surgery in this stage, but other treatments may help them live longer.
- Stage 4: This is the most advanced stage and the cancer has spread through the body. Stage 4 epithelioid mesothelioma patients have fewer treatments available, but long-term survival could still be possible.
The other types of mesothelioma (such as peritoneal) don’t have official stages, but doctors can assess cancer spread to determine the best treatment plan.
It may be possible to become a long-term survivor, even with late-stage or metastatic epithelioid mesothelioma, by getting treatment.
Is epithelioid mesothelioma curable?
While there’s no universal cure, some patients have achieved long-term remission from epithelioid mesothelioma with medical treatment from top specialists.
Get a Free Veterans Packet to learn more about treatments that could possibly help you recover or live longer from epithelioid malignant mesothelioma.



